Tag Archives: Hyperuricemia
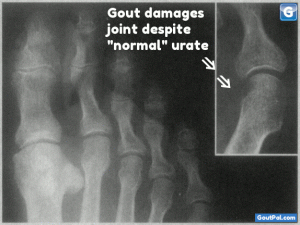
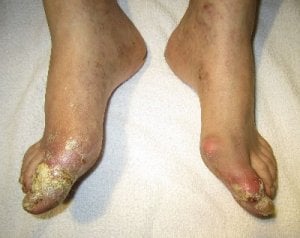
What’s new with hyperuricemia? People say excess uric acid isn’t dangerous. Why wait until it destroys your joints? Get the latest news on hyperuricemia.
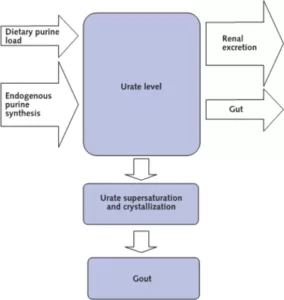
Hyperuricemia is the medical term for excess uric acid. When you understand hyperuricemia, you understand your gout better. Also, you are better placed to discuss gout with your doctor and other medical professionals.
This blog shows my updates and news about the hyperuricemia guidelines. For more information, please see the hyperuricemia guidelines.