Hot on the heels of yesterday’s article about fixing gout by stopping medications for other diseases, I present a completely different aspect of other diseases.
Our doctors speak of co-morbidities when gouty arthritis is accompanied by other diseases. Statistically, it is common for gout sufferers to have higher than average high blood pressure, heart disease, and other conditions. Now, I’m not suggesting that falling prey to additional diseases is good for gout. But just as we saw yesterday that some medicines can cause gout, we now know that some medicines for common diseases can also help gout patients.
Back in 2007, I reported on losartan, a medicine for high blood pressure, as a uric acid lowering treatment[1].
losartan, decreases SUA level, whereas other ARBs, such as candesartan, have no lowering effect.
Since then, more research has been done in this area, to the point where gout specialists are now listing losartan as a gout treatment (and I will follow suit, and add it to the gout treatment section in due course).
Three significant reviews recently included losartan as a uric acid lowering medicine.
Drugs that raise
serum urate concentrations
- Diuretics
- Tacrolimus
- Ciclosporin
- Ethambutol
- Pyrazinamide
- Cytotoxic chemotherapy
- Ethanol
- Salicylates (low dose)
- Levodopa
- Ribavirin and interferon
- Teriparatide
Drugs that lower
serum urate concentrations
- Ascorbic acid
- Benzbromarone
- Calcitonin
- Citrate
- Oestrogens
- Fenofibrate
- Losartan
- Probenecid
- Salicylates (high dose)
- Sulfinpyrazone
| Tying in with yesterday’s review of bad medicines for gout, the British medical journal, The Lancet, published handy lists of the bad and the good in their Gout Seminar[2]. |
In the USA, gout experts, Schumacher & Weaver, have included switching medicines as one of their core principles for managing gout[3]:
medications that raise SUA should be avoided or their use limited. For example, diuretics are a common risk factor for gout. For patients with both gout and hypertension, replacing a thiazide diuretic that increases SUA with the angiotensin II receptor antagonist losartan, a uricosuric that inhibits URAT-1, may lower both blood pressure and SUA.
For patients with gout and hyperlipidemia, replacing their lipid-lowering agent with fenofibrate, which has been shown to have uricosuric SUA-lowering effects in a double-blind, placebo-controlled, crossover RCT, may be helpful.
Many gout patients are on low-dose aspirin because of their cardiovascular comorbidities, but aspirin at low doses ( 3 g/day). A recent study reported that using low-dose aspirin (
Schumacher, this time with Baker, repeated similar advice, more succinctly, last year in their Update On Gout and Hyperuricemia[4]:
Losartan, fenofibrate, statins, vitamin C and increased coffee intake have all been shown to modestly increase urine uric acid excretion. There are currently no data in regard to the clinical utility of these interventions alone in the treatment of hyperuricemia and gout. However, consideration of hyperuricemia when choosing between blood pressure and cholesterol treatments may be appropriate and helpful in many patients.
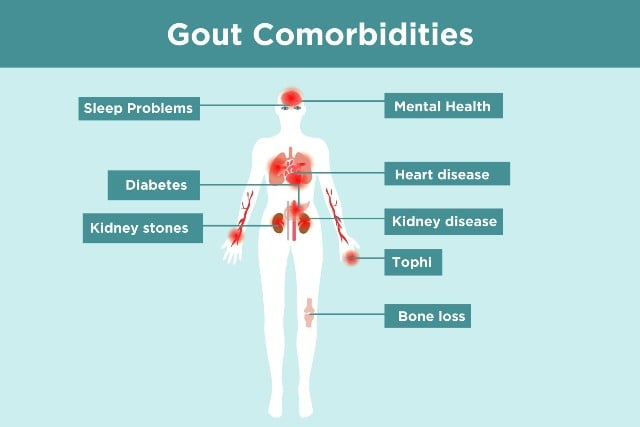
So, if you are a gout patient being treated for other conditions, now is the time to talk to your doctor about possible alternative medicines. Then tell us how you got on, in the gout forum.
Cure Gout With More Disease References
- Iwanaga, Takashi, Masanobu Sato, Tomoji Maeda, Toshio Ogihara, and Ikumi Tamai. “Concentration-dependent mode of interaction of angiotensin II receptor blockers with uric acid transporter.” Journal of Pharmacology and Experimental Therapeutics 320, no. 1 (2007): 211-217.
- Richette P, Bardin T. “Gout.” Lancet. 2010 Jan 23;375(9711):318-28.
- H. Ralph Schumacher, Jr., MD, Arthur L. Weaver, MD, MS, FACP, MACR. “A Specialty Monograph Focusing on Core Principles in the Diagnosis and Management of Gout and Hyperuricemia.” University of Pennsylvania School of Medicine and TCL Institute (2009). See Gouty Tophi & Bone Erosion.
- Baker, J. F., and H. Ralph Schumacher. “Update on gout and hyperuricemia.” International journal of clinical practice 64, no. 3 (2010): 371-377.
Cure Gout With More Disease Document Change History
 To read the document change history, click the GoutPal History image on the right.
To read the document change history, click the GoutPal History image on the right.
Do you have suggestions for improving Cure Gout With More Disease? Then, please send your idea using the Feedback Form, below.
Please give your feedback
Did this page help you? If yes, please consider a small donation. Your donations help keep GoutPal's gout support services free for everyone.
If not, please tell me how I can improve it to help you more.
- YouTube
- The gout forums.